Last updated: 17/06/20
First published: 30/03/20
Contents:
- Introduction
- Principles and values
- Strategic Commissioning
- Collaboration and Communication
- Sector funding and support
- Business continuity plans
- Cashflow
- Retrospective reconciliation
- Care and Support at Home (including domiciliary care, supported living & extra care and housing support)
- Residential care
- Workforce availability
- Sick Pay
- Rapid adjustment of support
- Infection control
- Use of non-contracted providers
- Other useful information
- Appendix 1: Legislative changes of the Coronavirus Act 2020 on the Social Services and Well-being (Wales) Act 2014
1. Introduction
This guidance note has been co-produced by the Association of Directors of Social Services (ADSS) Cymru, Care Inspectorate Wales (CIW), Social Care Wales, the Welsh Local Government Association (WLGA) and Welsh Government; and is for health board and local authority commissioners.
This is a second iteration of our guidance and it has evolved through the management of the COVID-19 outbreak. While it captures developments over the last couple of months, we acknowledge that other issues will emerge and that guidance linked to within this document may change. We would therefore expect to supplement this guidance again in the light of such issues, and advise all commissioners to ensure they are accessing the most-up-to-date guidance.
The guidance was initially designed to summarise the pressures being placed on children and young people’s and adults’ social care providers in Wales arising from the COVID-19 outbreak and examine possible ways in which commissioners could mitigate them.
However, as we move out of the initial critical phase of the pandemic, it is an opportunity to explore ways of supporting integrated resilience and recovery planning more holistically and ensure we refocus on the key principles and values set out in A Healthier Wales[1].
This guidance comes from a shared ambition to ensure providers are supported to maximise availability of care and support and to remain operationally and financially resilient, not just in the short-term but in the long-term as well. Social care & support services are part of our whole health and care system. Therefore, based on A Healthier Wales, we want to reiterate our shared ambitions, principles and values in relation to our support for these providers during the response to COVID–19:
- Commissioning health and social care services seamlessly – in each region of Wales the health and social care system will work together to plan, secure and fund sustainable services that provide a seamless experience and better health and wellbeing outcomes for people;
- All partners working together as equal partners – to make our services work as a single system, we need everyone to work together openly and transparently;
- Sharing information to support better collaborative decision-making – Seeing the service user as a whole and planning to support their health and wellbeing outcomes collectively;
- Transferring people and services safely from hospitals to communities; ensuring that promoting recovery becomes ‘everybody’s business.’
- Ensuring parity of esteem between the health and care workforce in Wales, so that every service is a safe and rewarding place to work.
This guidance does not deal with issues of infection control, which can be accessed separately here. Rather, it focusses on what commissioners should be considering and what they can do to support providers, in the knowledge that Welsh Government and other organisations such as Care Inspectorate Wales and Social Care Wales are also giving their own guidance and mitigation to support the sector at this time.
We describe these actions as what commissioners “can” do because our shared expectation is that commissioners actively consider all these issues and possible mitigating measures and do what is right and necessary to support their local providers. We also recognise they will be working with their local providers and county voluntary councils (CVCs) on a collaborative basis to identify issues and agree actions and mutual expectations.
In addition to the time-limited legislative changes made to social care in Wales by the UK Government’s Coronavirus Act 2020, the Welsh Government has worked with regulators to ease some of the requirements placed on providers, particularly those relating to the Regulation and Inspection of Social Care (Wales) Act 2016, to give them the scope to flex and adapt to changing circumstances they might encounter in dealing with the virus and its impact. Again, these changes are time-limited and will be reviewed.
Further information on the legislative changes of the Coronavirus Act 2020 on the Social Services and Well-being (Wales) Act 2014 can be found at Appendix 1:
While there is a significant focus on the impact of COVID-19 on adult social care settings, much of this guidance in relation to commissioning principles, values and best practice approaches, apply equally to children’s services.
Welsh Government has issued COVID-19 operational guidance for children’s social services, which should be read in conjunction with this guidance.
This is a second iteration of our guidance and it has evolved through the management of the COVID-19 outbreak. While it captures developments over the last couple of months, we acknowledge that other issues will emerge. We would therefore expect to supplement this guidance again in the light of such issues.
2. Principles and Values
While the Coronavirus Act 2020 has made some time-limited modifications to the Social Services and Well-being (Wales) Act 2014, the overarching principles of the Social Services and Well-being Act still remain:
- Prevention and Early Intervention – minimising the escalation of critical need;
- Voice and Control – the individual and their needs are front and centre;
- Co-production – encouraging individual design and delivery of care.
These should continue to be core guiding principles. However, it is clear commissioners and care providers are facing rapidly growing pressures as more people need support because family / Carers are unwell or unable to reach them, and as care workers are having to self-isolate or are unable to work for other reasons. Therefore, any planning or decision-making relating to services in this public health emergency must be underpinned by an additional framework of support.
In addition to the A Healthier Wales values and principles set out in the introduction, the Welsh Government’s guidance on Adult Social Services during the COVID-19 Outbreak also highlights the Ethical Framework for Social Care, whichall four administrations in the UK have signed up to and must be a key component of the planning and decision-making process of commissioning services.
3. Strategic Commissioning
In these challenging times, rapid response and adjustments to service delivery become the immediate priority for commissioners. However, it is vital that commissioning organisations and commissioners continue to protect capacity to consider the wider aspects of strategic commissioning and the commissioning cycle (see fig 1). Commissioners have a responsibility to effectively analyse supply and demand patterns and plan to secure appropriate service provision to match. The COVID-19 surge, in both demand and capacity, will hit different parts of the health and social care system at different times. It is essential that commissioners are effectively gathering and analysing data to help them plan effectively for the short, medium and longer term.
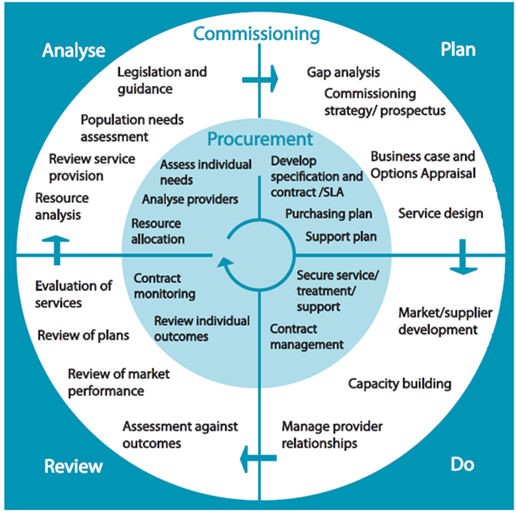
Fig 1 – Institute for Public Care (IPC) commissioning cycle
4. Collaboration and Communication
To plan and deliver services during a time of crisis and uncertainty requires openness, trust and the sharing of resources where possible. Commissioners and providers should seek to maximise their collective expertise, talent and experience and collaborate to find the right solutions for service users and their workforce. Central to this is the need for effective and responsive channels of communication.
Providers face a fast-moving and uncertain operational environment and we anticipate pressure on services to increase in the coming weeks and months ahead. Therefore, they will need the ability to raise issues and get answers quickly, and to be able to solve problems collaboratively, both with commissioners and with each other.
We would strongly recommend that a local open book dialogue is had to build trust between providers and commissioners. Having transparent, two-way conversations with providers at the earliest possible stage will afford them the opportunity to bring their experience and expertise to the fore and will help inform the commissioning, planning and decision-making process. Moreover, having regular and routine ‘face-to-face’ discussions/meetings with providers (using appropriate IT platforms where possible) will further facilitate relationship confidence and will ensure any barriers to operational delivery are addressed in a timely manner.
Recommended actions:
Action | Who |
Ensure effective two-way communication:
|
Local authorities in conjunction with local health boards – ideally this would be collated on a regional partnership board (RPB) level where appropriate and linked into local resilience forums (LRF)
|
ADSS Cymru to co-ordinate and produce a weekly service update bulletin on behalf of national partner agencies (Welsh Government, Public Health Wales, Social Care Wales, Care Inspectorate Wales, Welsh Local Government Association) and for Care Inspectorate Wales to issue the communication to providers. The bulletin, along with previous additions will be hosted on the ADSS Cymru website. | ADSS Cymru, National Commissioning Board, WG and Care Inspectorate Wales (CIW). |
Share infection control policy & procedures and training materials (including access to online training) with providers to ensure policy and practice follow up-to-date advice and guidance. | PHW, HEIW, SCW & ADSS Cymru (weekly bulletin). |
Provide information (e.g. FAQs) and guidance for informal carers, direct payment recipients and their personal assistants and self-funders (providers and third sector organisations will be able to assist with dissemination). This should include points of contact in the event that individual care arrangements break down. | Social Care Wales |
5. Sector Funding and Support
The Welsh Government has announced several packages of financial support to help the sector during this first phase of managing the impact of the pandemic:
- Independent Sector – Business Wales has developed a suite of information and guidance on a range of COVID-19 related issues. This includes a series of webinarscovering topics like alternative business models and diversification, cashflow and accessing finance, HR policies and procedures, including employment law, sick pay and zero-hour contracts, managing teams and workload remotely, encouraging productivity and negotiating with suppliers and customers.
The Welsh Government Economic Resilience Fund (ERF) Phase 1, was closed to further applications at the end of April. However, ERF Phase 2 has been launched (9 June) and non-VAT registered companies will be able to apply. Information on the scheme can be found here and the ERF Eligibility Checker can be found here.
- Third Sector - £24m Third Sector Resilience Fund, to promote volunteering and develop further sector capacity to aid local community responses to the pandemic. Plus, additional capital flexibility through the Community Facilities Programme, to allow the purchase or replacement of equipment to support the COVID-19 response.
Further support and information is also available from the WCVA website or more locally from Third Sector Support Wales’ members.
Funding advice is also available on the Funding Wales online portal.
- Public Sector – The Welsh Government has announced an additional £10m of funding to Wales’ health and social care organisations to help get those recovered from COVID-19 home sooner. This will fund new and enhanced home care packages to support patients to leave hospital for their on-going assessment and recovery. It will also help fund crucial community services supporting the COVID-19 response that are helping people to stay at home safely.
Welsh Government has also announced a £40m ring-fenced, cross-sector fund for adult social care, which has been included in the COVID-19 Local Government Hardship Fund. It is to help address the reasonable, additional costs (March to June 2020) resulting directly from the pandemic that adult social care providers are experiencing in order to maintain their care provision and be able to respond to any additional demand for care which arises.
A guidance document was circulated by Welsh Government (27 April) to clarify the purpose for the funding. The fund does not cover:
- additional costs arising in relation to healthcare (CHC, FNC)
- lost income from self-funders
6. Business Continuity Plans
Good business continuity planning assists resilience. Ensuring service continuity will require collaborative working and flexibility of all partners, adhering to the key principles and values set out above.
Commissioners should avoid simply asking care providers to submit their own business continuity plans (BCPs) or requiring them to submit business resilience data / information, unless there is an intention to analyse the information collaboratively and offer constructive guidance and support. BCPs should be the starting point between providers and commissioners to identify service resilience and continuity risk and which aspects need further work or support. Where possible such analysis should be undertaken at a regional / national level and shared e.g. Children’s Commissioning Consortium Cymru (4Cs) are collating and analysing residential and fostering framework providers.
There should also be a recognition that some aspects of the continuity plans rely on support from other organisations within the local resilience forum (LRF) community.
Commissioners can also help providers by ensuring they share their own local resilience/ reprioritisation plans, and by ensuring that providers are linked into the wider considerations and plans of LRFs, such as distribution of PPE, access to testing, childcare, school and transport services.
Recommended actions:
Action | Who |
Identify mutual support opportunities (internal and external partners): - Commissioners to establish contact procedures and data sharing arrangements with providers, enabling reduced and focused contact across agencies e.g. EHO, PHW, LA and HB (linked to escalation framework and support detailed above);
| Providers, local authorities’, and local health boards – ideally this would be collated on an RPB level where appropriate and linked into LRF.
|
Local authorities and local health boards can co-ordinate deployment of non-practicing experienced health and social care staff within a region across statutory and independent sectors. This needs to link in with the Wales-wide approach through the ‘WeCare Campaign’ where there is a ‘regional connector’ identified in each region supporting this for social care. There is also a free jobs portal to advertise vacancies. Longer term planning principles should be applied. For example, even though there may not be an immediate workforce gap or shortage, communication should be maintained with people seeking to enter the social care workforce with a view to engaging them in training and development opportunities, enabling them to enter the workforce, as and when, the need arises. | |
Provide guidance for providers in regard to safer recruitment procedures; this now includes guidanceon volunteer recruitment produced with WCVA. | Social Care Wales, CIW & DBS. |
Establish standard operating procedures across partners (commissioners, regulators etc) for obtaining data on service continuity, with the principle of ask once’, and share wherever possible. | All public service agencies. |
Care Inspectorate Wales to contact individual providers directly ‘telephone check-in’ on a fortnightly basis to inquire about any specific challenges, pressures or concerns related to the operational delivery of their service and how further support can be provided if required. Feedback generated will be used to develop guidance and advice through their FAQ’s section on the website. | CIW to lead, liaising with local authorities and health boards. |
Share information about local innovations e.g.
| Regional Partnership Boards, The National Commissioning Board and National Commissioning Group can support identifying and sharing innovations. |
Commissioners should now be planning for: - Sustainability; maintaining critical services adversely affected by COVID (implementing escalation & support frameworks including workforce deployment, with standard operating procedures for distribution of PPE & streamlined testing pathways in closed settings). This links to Local Authority duties under section 144B of Regulation & Inspection of Social Care (Wales) Act 2016 - Resilience (in event of future spikes) and planning based on modelling for new types of need / demand for services);
- Recovery; reinstate and right-size including:
|
Local authorities in conjunction with local health boards (planners, lead allied health professionals) – ideally this would be collated on a regional partnership board (RPB) level where appropriate and linked into local resilience forums (LRF)
|
7. Cashflow
Commissioners should be discussing with providers whether there are any changes taking place that have an impact on provider operational and financial resilience. Requests from commissioners about information from providers about people who fund their own care may be particularly sensitive and should be accompanied by clear advice on why so doing would not be a breach of the General Data Protection Regulation (GDPR).
Invoice generation will become an increasingly complex activity. Providers will be focused on delivering support to people and managing sickness absence in their own workforce.
Providers may face additional financial sustainability challenges related to loss of income due to voids (residential / supported living / fostering services) and reduced delivery due to staff shortage, and this will be more acutely felt by smaller providers in the market who will have limited reserves to draw from.
Providers will also be facing unanticipated additional costs such as increased use of agency staff, increased liability for statutory sick pay, additional use of personal protective equipment (PPE including specialist PPE), and increased cost of liability insurance.
Recommended actions:
Action | Who |
Commissioners should make every effort to prioritise payment to social care providers and establish flexible arrangements such as:
| Local authorities and local health boards. |
Mitigate risks by:
| Local authorities and local health boards – ideally this would be a consistent approach at a RPB level where appropriate. |
Qualify and quantify additional costs of provision and make fee adjustments / temporary uplifts where possible and necessary. | |
Share local innovations, e.g.
| The National Commissioning Board and National Commissioning Group can support with sharing innovations. |
Provide formal written communication to providers detailing variations (to regulation / guidance / contracts) permitted during this emergency planning period, e.g.
| CIW, Social Care Wales, commissioners, including local authorities and local health boards / trusts |
8. Retrospective reconciliation
It is understandable that providers will have concerns about the implications of retrospective reconciliation. However, reconciliation is appropriate when actual levels of support differ markedly from what was planned. Yet, commissioners should be mindful of all the extra costs incurred by providers during this period, and of problems they may face in reducing variable costs in such a volatile operating environment. Providers should be mindful that, where actual support levels are significantly below plan, commissioners may have needed to fund support elsewhere.
How the discussions and process is handled is absolutely crucial. Commissioners must handle it sensitively, transparently and through open, two-way discussion, rather than unilateral imposition. The earlier that providers are engaged in such discussions, the better the likely outcome for both parties. The principles and values highlighted above must underpin those discussions and any approach taken so that relationship trust and confidence can be maintained, and provider reassurance secured.
9. Care and Support at Home (including domiciliary care, supported living & extra care and housing support, Shared Lives and Foster Care)
Increased service demands and pressure will be put on care at home providers in the coming weeks and months ahead, particularly in relation to rehabilitating those post-COVID-19 patients who have spent long periods in hospital. In anticipation of this demand for extra services, the Welsh Government has announced an additional £10m of funding to Wales’ health and social care organisations to help transfer those who have recovered from COVID-19 home sooner (see section ‘Sector Funding and Support’). Further planning work is being undertaken to provide additional support and guidance to manage this next phase and that will be published shortly.
However, in the interim, ensuring cashflow to those providers in the market is extremely important, as reduced cashflow will especially impact care at home providers. Delays in invoicing, invoice disputes and non-payment of invoices will have a serious negative impact on providers’ cashflow and sustainability in an already fragile market and should be avoided.
Commissioners may also consider making retainer payments for providers who offer e.g. respite services, who cannot now offer those services.
Care at home workers are included in the testing criteria for NHS and non-NHS workers as they are ‘Coronavirus Critical Workers’. The Welsh Government has produced guidance on how commissioners and providers of supported accommodation should manage their settings during the COVID-19 outbreak.
It sets out the need for practical measures to ensure those living and working in supported accommodation settings have the support, resources and policies needed to protect themselves; and that they also have access to the facilities to enable adherence to public health guidance on hygiene and isolation and measures to mitigate the risk. Moreover, it highlights the need for the mental and physical resilience of people in supported accommodation settings to be considered and the importance of trauma informed practice.
In addition, the Welsh Government has also issued guidancefor dealing with people who are unwilling or unable to self-isolate or follow coronavirus lockdown instructions.
10. Residential Care
Cashflow can also affect care homes, and commissioners can again offer support by paying on the planned support for people in given care homes (e.g. extending payment terms during periods in hospital / NHS facilities, paying additional time after death to accommodate guidance on enhanced cleaning / waste disposal) and the reconciling for any adjustments due to deaths or other factors. This is even more important as occupancy levels may become more volatile, with potentially more voids due to discharge guidance and infection control measures. Commissioners can agree with local care homes what level of certainty in terms of planned payments will help them through this volatility.
Some care home providers may be reluctant to accept new residents, to support the transfer of residents back to the home from hospital or an NHS facility. They may also be required to instigate restrictions on residents such as self-isolation, which may deprive individuals of their liberty. In those cases, providers need to be supported with the right information and guidance so that the right decisions are made for the individual, such as those with dementia.
In relation to hospital discharge, all commissioners (local authorities and health boards) should be following the guidance on discharge that has been issued by Welsh Government and should support providers, wherever appropriate, to mitigate the risks of transferring an individual safely back into a care home. Similarly, Public Health Wales (PHW) has produced guidance on preventing COVID-19 among Care Home Residents and Managing Cases & Outbreaks in Residential Care.
The testing regime for care homes has been updated (20May) so that every care home in Wales can now access testing for residents and staff. Policy and guidance around the testing regime in Wales is developing rapidly, particularly with the implementation of ‘Test, Trace, Protect’ (TTP). The most up to date information will be found on the Welsh Government’s Coronavirus (COVID-19) Testing webpage.
11. Workforce availability
Providers will face higher workforce absence rates, through medically recommended shielding, self-isolation, sickness and family caring responsibilities. While national school closures have been implemented in Wales in line with the other UK nations, plans are in place to ensure the children of key workers (defined by the Welsh Government) are allowed to remain in school. As policy plans to unlock schools are being developed nationally, the operational delivery will be the responsibility of each Local Education Authority. Further information can be found here.
Care providers will need to be able to deploy their staff flexibly and to hire new staff quickly. They will face increased cost pressures from higher use of agency staff. CIW and Social Care Wales have worked with Welsh Government to amend and disapply some of the current regulations following the enactment of the Coronavirus Act 2020. Moreover, the DBS service has provided guidance regarding the work it is doing to support the fight against COVID-19.
The Wales Government has provided funding to Local Authorities (via Hardship Fund) to support social care providers with these additional costs. Commissioners can mitigate this through recognising and funding these extra cost pressures. They can also ensure their contracts allow flexibility for providers in hiring and deploying staff.
See also recommended actions in ‘Communication and Collaboration’ & ‘Business Continuity’ sections above.
Whilst the perception may be that furloughing staff will be unnecessary in the social care sector at present given the unprecedented strains on the services and staff shortages, certain situations may arise where staff are not required or are unable to work, which would allow Providers to apply to the UK Government’s Coronavirus Job Retention Scheme (CJRS). For example, where the staff member is in a high-risk health group or is shielding in accordance with Government guidance and remains away from the workplace.
If providers want to explore options available to them under CJRS, then any new claim must be made and submitted no later than 30 June 2020.
Detailed records should be kept as to the decision-making rationale adopted with regard to the necessity of placing staff on furlough, along with a breakdown of staff pay compared to public funding received and any reductions in placement or service user numbers.
The well-being of the workforce is also incredibly important at this time. Social Care Wales has developed a suite of resource information to support both the workforce, more generally and managers. This information is continually being updated and built upon.
12. Sick pay
Providers face increased cost pressures due to higher sickness absence rates among their workforce: they have to pay staff statutory sick pay (SSP) or make sickness payments at a higher level than SSP because they have a contractual sick pay scheme (also known as an ‘occupational scheme’), which offers workers payments above the basic minimum amount of SSP, which is £94.25 per week. Information on statutory sick pay rights can be found here.
Commissioners will generally have well established arrangements with each of their providers in place, with clear channels of communication. Commissioners should endeavour to do all they can to mitigate SSP cost pressures. They could, for example, assist with cashflow by agreeing a reasonable amount based on an assumed average sickness absence rate and paying up front, rather than awaiting detailed records of actual sickness taken and backfill provided, and agree reasonable and proportionate ways of later reconciliation. An assumed average rate may be informed by governmental planning assumptions, but commissioners should not wait for this if it is delaying necessary financial support.
Further detailed guidance from Welsh Government to assist providers as employers and their staff to address key COVID-19 issues, including:
- Sick Pay
- Certification
- What to do if an employee needs time off work to look after someone
can be found here.
13. Rapid adjustment of support
Support will have to be rapidly adjusted. People will be admitted to hospital, may be required to self-isolate and not access communal facilities including bathrooms and kitchens, care visits changed to meet the most urgent needs and some care and support will take longer due to infection control precautions and the availability of staff.
This means that rapid decisions will need to be taken about appropriate adjustments of care packages, with a clear decision-making process in place. It will also increase providers’ costs as it will require extra management time to make these adjustments. There is also likely to be a higher ratio of travel to contact time in home care due to the rapid reorganisation of rounds and rosters.
Commissioners can mitigate this firstly by agreeing with their providers on how to adjust packages in a timely and non-bureaucratic way, without requiring prior authorisation, but within agreed limits.
If commissioners choose to retain decision-making about changes to care packages themselves, they will need to have enough staff at the right level available to make these decisions rapidly and have simple processes in place.
Commissioners can also fund additional costs incurred from extra administration and increased travel times and visit lengths in non 24/7 support at home settings (associated with safely ‘donning & doffing’ PPE), and for extra administration costs.
14. Infection control
Providers will face extra costs through the need for:
- more PPE;
- enhanced cleaning, sanitisation and laundry;
- enhanced waste disposal arrangements;
- adopting different working patterns to minimise the spread of infection, e.g. zoning some staff within care homes, providing staff accommodation.
Providers may also face greater difficulty in obtaining infection control products, PPE, handwash and disposable hand towels, due to increased demand for them.
Any stocks of PPE or other equipment provided by Welsh Government and held by local authorities should be distributed in accordance with prioritised need and equitably across different segments of the adult, and children and young people social care sector.
Local Authorities can help this process by issuing clear instructions to their staff about:
- how to assess the total potential PPE demand across all social care providers in their area, and
- how such stocks should be made available to providers who need them (including 24/7 access) and what stocks (e.g. specialist equipment) are available from health boards.
PHW has issued advisory notes for the use of PPE in specific settings - in social care settings (Care Homes and Domiciliary Care) and in housing, health, social care support settings.
Commissioners should ensure that providers are aware of current guidance and have effective risk management procedures and arrangements to train, advise and support staff and ensure appropriate supplies in relation to:
- basic hygiene procedures including hand-washing;
- correct use of PPE, including correct items for each task, fit testing (where appropriate) ‘donning and doffing’ and safe disposal;
- how to escalate any concerns.
The following attached documents provide additional guidance on donning and doffing of PPE:
15. Use of non-contracted providers
Commissioners who contract with approved or ‘framework’ providers at fixed prices may also be looking to other non-contracted providers in the local area, as demand for care and support peaks. Consideration should be given to the potential impact of paying contracted providers at a lower rate than providers which are off-framework or off-contract.
Commissioners can mitigate this through careful consideration of the prices it pays for care and the available capacity in the local market; and should be mindful of longer-term impact on the market if there is more use of non-contracted providers.
Recommended actions:
Action | Who |
Commissioners may have to seek exception to contract and procurement regulations in order to contract with providers outside of usual contract frameworks / non-approved providers. | Local authorities and local health boards – ideally this would be consistent across an RPB area |
Commissioners should share due diligence information (registration, insurance levels, Dun & Bradstreet checks), etc with other commissioners in regards providers outside of usual contract frameworks / non-approved providers in their area that are approved elsewhere in Wales | The National Commissioning Board, National Commissioning Group and national commissioning units can support with sharing information. |
The National Commissioning Board in conjunction with National Commissioning Group and national commissioning units will provide support in regards monitoring market sustainability risks | The National Commissioning Board, National Commissioning Group and national commissioning units |
16. Other useful information
Prior to the public health emergency, ADSS Cymru produced detailed advice notes to support commissioners on developing integrated service models and pooled budgets which can be found here.
17. Appendix 1: Legislative changes of the Coronavirus Act 2020 on the Social Services and Well-being (Wales) Act 2014
Section 25 |
| Provision to clarify local authorities’ responses following a refusal of a needs assessment for an adult carer (but subject to requirements around abuse or neglect). |
| Paragraph 21 |
Section 32(1)(a) |
| Determination of whether needs meet the eligibility criteria. |
| Paragraph 22(2)(a) |
Section 32(2(b) |
| Determination of charge as part of determination of eligibility. |
| Paragraph 22(2)(b) |
Section 32(1) |
| Omission of English text relating to determination of whether needs meet the eligibility criteria. |
| Paragraph 22(3)(a) and (b) |
Section 32((2)(b) |
| Omission of Welsh text relating to determination of whether needs meet the eligibility criteria. |
| Paragraph 22(4)(a) and (b) |
Section 35 |
| Provision to clarify assessments can be undertaken and determination of eligibility made in order to meet needs of adult or adult carer. |
| Paragraph 23 |
Section 35(3)(a) |
| Omission of this sub-section. |
| Paragraph 26 |
Section 40 |
| Provision to clarify assessments can be undertaken and determination of eligibility made in order to meet needs of adult or adult carer. |
| Paragraph 23 |
Section 40(3) |
| Substitution of English text relating to conditions for meeting needs of adult carer. |
| Paragraph 27(a) and (b) |
Section 40(3) |
| Substitution of Welsh text relating to conditions for meeting needs of adult carer. |
| Paragraph 27(b) |
Section 54 and section 55 |
| Provision to clarify local authorities do not have to comply with duties to prepare a care and support for an adult or a support plan for an adult carer and relevant aspects of the associated regulations under section 55. |
| Paragraph 31 |
Section 56 |
| Provision to clarify that local authorities do not have to comply with duties relating to portability of care and support during the emergency period. |
| Paragraph 32 |
Section 56 |
| Provision also made in relation to portability of care and support for the period following the emergency period. |
| Paragraph 33 |
Section 57 |
| Provision to clarify that local authorities do not have to comply with duties where person expresses a preference for particular accommodation. |
| Paragraph 29 |
Section 63(2) |
| Provision to clarify local authorities’ responsibilities to carry out a financial assessment before imposing a charge for meeting needs of adult or adult carer under sections 35 or 40 and for charging for meeting needs during an emergency period. |
| Paragraphs 25, 28 and 30 |
[1]Welsh Government, A Heathier Wales: our Plan for Health and Social Care, https://gov.wales/sites/default/files/publications/2019-10/a-healthier-wales-action-plan.pdf




